10 Nursing Assessment Red Flags Every Nurse Must Recognize
Patient assessment is one of the most basic duties of nurses. During this process, nurses must identify red flags indicating critical or life-threatening conditions.
In Indonesia, nurses work in various settings, including tertiary hospitals, emergency units, puskesmas, clinics, and community outreach. This emphasizes the importance of early recognition of clinical red flags to prevent deterioration, lower complications, and save lives.
Understanding these 10 critical nursing assessment red flags is essential for prompt recognition and rapid response, ensuring patient safety.
1. Sudden Onset Chest Pain
Sudden chest pain, especially when paired with sweating, nausea, pain radiating to the arm or jaw, or shortness of breath, is a significant red flag.
❓Possible causes: myocardial infarction, unstable angina, and aortic dissection
✅Nursing Actions:
1. Act quickly to stabilize the patient and enable rapid diagnosis and treatment, empowering nurses to act decisively.
2. Escalate the situation, perform an ECG, check vital signs, and provide oxygen as needed.

2. Severe Shortness of Breath or Labored Breathing
Respiratory distress is one of the most urgent nursing assessment red flags.
Look for:
1. Use of accessory muscles
2. Cyanosis
3. Inability to speak complete sentences
4. Low oxygen saturation
❓Possible causes: asthma exacerbation, pneumonia, anaphylaxis, pulmonary edema, or pneumothorax.
✅Nursing actions:
1. Ensure airway patency
2. Administer oxygen as indicated
3. Monitor respiratory status closely
4. Escalate immediately
3. Altered Level of Consciousness
Any sudden change in consciousness—from confusion and drowsiness to unresponsiveness—requires rapid attention.
❓Possible causes: Hypoglycemia, Stroke, Infection or sepsis, Drug or toxic substance exposure
✅Nursing actions:
1. Assess using GCS or AVPU
2. Check blood glucose
3. Monitor neurological status
4. Notify the medical team immediately
4. Uncontrolled Bleeding
Active bleeding, whether internal or external, can quickly lead to shock.
❗Warning signs:
1. Hypotension
2. Tachycardia
3. Pale, cool skin
4. Anxiety or restlessness
✅Nursing actions:
1. Apply direct pressure
2. Monitor vital signs for shock
3. Prepare for urgent intervention or referral
5. High Fever with Rash or Stiff Neck
The combination of fever, rash, and neck stiffness may indicate meningitis or sepsis, both of which require emergency care.
✅Additional signs to look for:
1. Petechial rash
2. Severe headache
3. Photophobia
6. New Neurological Deficits
Sudden neurological changes are among the most time-sensitive red flags in nursing assessment (Ernstmeyer & Christman, 2021).
Examples: facial drooping, arm weakness, slurred speech, loss of balance, sudden severe headache
✅Use the FAST tool to screen for potential stroke. A widely used and easy-to-remember acronym to quickly identify the most common signs of a potential stroke and emphasize the importance of rapid action.
❗Understanding the FAST tool is crucial as it provides a quick, easy method to identify stroke signs and act swiftly.
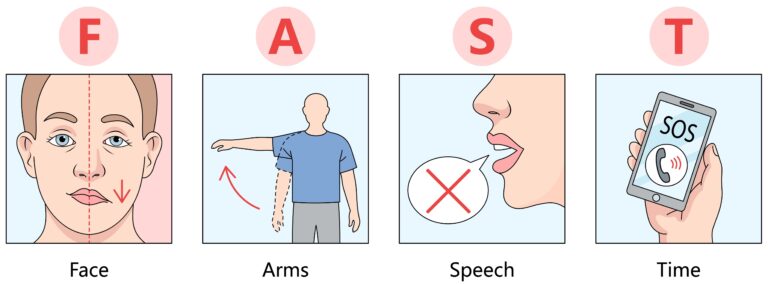
F = Face drooping or twisting
One common symptom of a stroke is that half of the face droops or slightly twists downward.
Ask the person to smile.
What to look for: Does one side of the face droop, or is it numb? Is the person’s smile uneven?
A = Arm weakness
Ask the person to raise both arms.
Does one arm drift downward, or is one arm unable to be raised fully?
When experiencing arm weakness, one arm might be weak or numb. Does one arm drift downward, or is one arm unable to be raised fully?
S = Speech difficulty
Ask the person to repeat a simple phrase.
Is their speech slurred, or do they struggle to find words or understand what you say?
Slurred speech, word switching, and difficulty speaking clearly are also normal signs of a stroke.
T = Time to call emergency services (Indonesia 112)
On average, 1.9 million brain cells die every minute that a stroke is untreated.
If you notice any of these symptoms, even if they go away, call for emergency medical help immediately. Time is critical, as early treatment can save lives and improve outcomes. Remember the time the symptoms first appeared or when the person was last known to be well.
Early stroke treatment increases the chances of survival and reduces disability rates (Yamanie et al., 2025).
7. Acute Abdominal Pain with Guarding or Rigidity
This may indicate life-threatening abdominal conditions such as:
1. Appendicitis
2. Peritonitis
3. Bowel obstruction or perforation
4. Ectopic pregnancy
✅Look for signs of distention, rebound tenderness, persistent vomiting, or hypotension.
8. Sudden Drop in Blood Pressure
A quick drop in blood pressure can be caused by:
1. Sepsis
2. Internal bleeding
3. Cardiogenic shock
4. Anaphylaxis
✅Always monitor trends—sudden changes are riskier than a single low reading.
9. Decreased Urine Output (<30 mL/hour)
Oliguria is an early red flag for (Manu et al., 2024):
1. Acute kidney injury
2. Dehydration
3. Sepsis
4. Poor perfusion/shock
✅Nursing actions:
1. Monitor intake and output
2. Assess hydration status
3. Report promptly
10. Severe Pain Disproportionate to Examination
If a patient’s pain is much greater than what the physical findings suggest, be cautious.
❗Possible emergencies include:
1. Compartment syndrome
2. Necrotizing fasciitis
3. Ischemia
4. Aortic aneurysm rupture
✅This red flag is often overlooked. Severe pain that does not match physical exam findings can be missed because clinicians may too often rely on objective signs to confirm a patient’s history. Meanwhile, serious underlying conditions, like ischemia, may initially show subtle or absent physical signs.
General Actions Nurses Must Take When Red Flags are Observed

Whenever a nursing assessment red flag is identified, nurses should take the following actions immediately:
1. Ensure Airway, Breathing, and Circulation (ABC) are Stable
Check airway patency
Assess breathing effort, rate, and oxygen saturation
Monitor circulation: pulse rate, blood pressure, skin color, capillary refill
❗If unstable → escalate immediately.
2. Position the Patient Safely
Breathing issues → High Fowler’s/upright position
Hypotension/fainting → Supine with legs elevated (unless contraindicated)
Suspected stroke → Head elevated 30 degrees
✅Correct positioning reduces the risk of deterioration.
3. Administer Oxygen if Indicated and Allowed by Protocol
Use a nasal cannula or mask based on severity
Titrate to maintain appropriate SpO₂
Monitor continuously
✅Oxygen is a first-line intervention for most emergency symptoms. (Weekley & Bland, 2025)
4. Monitor Vital Signs Frequently
Take and re-check:
Blood pressure, heart rate, respiratory rate, SpO₂, temperature, level of consciousness (AVPU/GCS)
✅Repeat every 5–15 minutes, depending on severity.
5. Establish or Maintain IV Access
For rapid medication, fluid resuscitation, or lab draws.
6. Prepare Emergency Equipment and Medications
Depending on the scenario:
1. Suction machine
2. Bag-valve-mask (BVM)
3. Defibrillator/AED
4. Nebulizers
5. Epinephrine (anaphylaxis)
6. IV fluids
❗Anticipate what may be needed.
7. Conduct a Focused Assessment Based on the Red Flag
Examples:
Chest pain → ECG, chest auscultation
Shortness of breath → lung assessment, respiratory pattern
Altered mental status → glucose check, neurological exam
Uncontrolled bleeding → locate source, apply pressure
✅This step supports rapid diagnosis.
8. Notify the Physician or Emergency Team Immediately (SBAR)
Use clear communication:
Situation: What is happening now
Background: Relevant medical history
Assessment: What you found
Recommendation: What you need urgently
✅This ensures rapid escalation.
9. Prepare for Possible Emergency Transfer or Activation of Code Team
Examples:
Activate emergency response / RRT
Call 112 if in a community setting
Prepare the patient for ER transfer or advanced care
❗Time lost = outcome worsens.
10. Provide Psychological Support and Reassurance
Stay with the patient
Speak calmly
Reduce anxiety and unnecessary movement
Explain what you are doing
✅Anxiety increases oxygen demand and worsens symptoms.
11. Document Assessment, Interventions, and Patient Response
Record precisely:
Symptoms observed
Vital signs
Interventions performed
Time and sequence of events
Provider notifications
✅Accurate documentation supports continuity of care and legal protection.
❗Disclaimer:
The actions outlined above represent general steps that nurses may take when encountering nursing assessment red flags. These recommendations should not replace local clinical guidelines, institutional policies, standing orders, or the direction of a licensed medical provider. Each healthcare facility may have specific protocols for emergency response, oxygen administration, medication preparation, documentation standards, and escalation pathways. Nurses should always follow their facility’s SOPs, scope-of-practice regulations, and the instructions of the attending physician or emergency medical team. Clinical judgement and situational assessment remain essential in all patient care decisions.
📖Read more about patient assessment in the nursing process in our previous blog.
Recognizing nursing assessment red flags is a core competency that greatly enhances patient safety and clinical decision-making. When nurses detect these early warning signs, they help prevent complications, facilitate timely medical interventions, and improve patient outcomes.
🩺Prepare to enhance your clinical assessment skills!
Join Zafyre’s Patient Assessment training designed to meet current clinical standards and Kemenkes competency requirements.
ENROLL NOW
References:
1. American Heart Association (AHA). (2025). Check out the F.A.S.T. Experience. Www.stroke.org. https://www.stroke.org/en/fast-experience
2. Bacelar, L., de Jesus Meszaros, M., de Freitas Neves Silva, M., & São‐João, T. M. (2023). Nursing Training for early clinical deterioration risk assessment: Intervention Protocol (Preprint). JMIR Research Protocols, 12(1), e47293–e47293. https://doi.org/10.2196/47293
3. Ernstmeyer, K., & Christman, E. (2021). Chapter 6 Neurological Assessment. National Library of Medicine; Chippewa Valley Technical College. https://www.ncbi.nlm.nih.gov/books/NBK593206/
4. Manu, Tantakoun, K., Zara, A. T., Ferko, N. C., Kelly, T., & Dabrowski, W. (2024). Urine output is an early and strong predictor of acute kidney injury and associated mortality: a systematic literature review of 50 clinical studies. Annals of Intensive Care, 14(1). https://doi.org/10.1186/s13613-024-01342-x
5. Payton, H., & Warren, S. (2024). How to identify red-flag symptoms and refer patients appropriately. The Pharmaceutical Journal, 312(7983). https://doi.org/10.1211/pj.2024.1.305174
6. Registeredbsn.com. (2023, July 15). RB.S.(n) Clinical Pearl: Nursing Assessment Red Flags. Registered B.S.n. https://www.registeredbsn.com/nursing-assessment-red-flags/
7. Saharuddin, S., Nurachmah, E., Masfuri, M., Gayatri, D., Kimin, A., Sakti, M., Saidi, S. B., & Yona, S. (2025). Exploring Clinical Decision-Making Competencies of Emergency Nurses in Trauma Care in Indonesia: Qualitative Study. Asian Pacific Island Nursing Journal, 9. https://doi.org/10.2196/74282
8. Weekley, M. S., & Bland, L. E. (2025). Oxygen Administration. National Library of Medicine; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK551617/





