Non-Drug Pain Relief Techniques Every Nurse Should Know

Introduction: Pain Control Is More Than Medication
Pain is one of the most common reasons why patients seek care. May it be in emergency rooms, maternity wards, surgical units, or community health centers. For nurses, pain management is not just a task. It is a daily clinical responsibility. It directly affects the recovery, safety, and satisfaction of patients.
For many years, the primary solution for pain has been medications, especially opioids. Today, our healthcare system is already shifting to much safer and balanced practices. Multimodal techniques, both drug- and non-drug, are emphasized by international organizations like the World Health Organization (WHO). These techniques aim to lessen side effects and enhance patient outcomes.
In Indonesia, national health regulations and nursing standards support comprehensive pain management that includes non-pharmacological approaches. This aligns with Perawat’s scope of practice under Permenkes No. 26 of 2019 and clinical expectations of the Standar Profesi Perawat — where nurses are responsible for assessment, planning, intervention, and evaluation of patient pain using both drug and non-drug methods.
Simple non-drug pain relief techniques frequently offer the quickest and safest comfort — sometimes even before pharmaceuticals are required — because nurses are the ones who are closest to patients around-the-clock.
This article explores the essential non-drug pain relief techniques every Indonesian nurse should know and how to apply them effectively in daily practice.
What Is Non-Drug Pain Management?
Non-pharmacological pain management (NPPM) or non-drug pain management refers to interventions that reduce pain without the use of medications (Tsegaye et al., 2023).
✔️Non-drug pain relief techniques work by:
1. Reducing inflammation
2. Relaxing muscles
3. Improving circulation
4. Lowering anxiety and stress
5. Modifying pain perception in the brain
✔️These are commonly used to:
1. Reduce patients’ reliance on medications
2. Enhance patients’ sense of control and comfort
3. Improve outcomes in mild to moderate pain
4. Support recovery in procedures, chronic pain, and post-operative care
5. Integrate smoothly into holistic nursing care
Unlike medications that may cause side effects such as drowsiness, nausea, or respiratory depression, these are low-cost, safe, and nurse-driven techniques.
It is important to note that non-drug pain relief techniques complement pharmacologic management — they do not replace needed medication but enhance its effectiveness and support patient-centered care.
Why Non-Drug Pain Relief Techniques Matter in Indonesian Healthcare
In Indonesia, non-drug pain management is particularly important for several practical reasons:
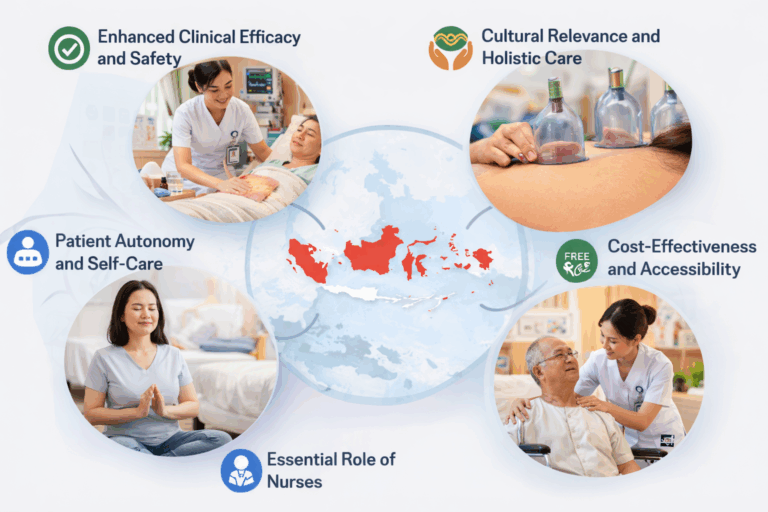
1. Enhanced Clinical Efficacy and Safety
•Complementary Approach: Non-drug techniques do not replace medication but work alongside it to provide more effective pain relief.
•Reduced Side Effects: By using these techniques, healthcare providers can reduce the dosage of analgesic drugs needed, thereby minimizing side effects associated with long-term medication use.
•Proven Results in Infants: Studies in Indonesia have shown that techniques like sensory saturation with breastfeeding (SSB) are highly effective in reducing pain intensity in neonates. Similarly, the Yakson method (a traditional Korean technique) and Gentle Human Touch have been shown to reduce pain and stabilize heart rate in premature infants significantly (Fitri et al., 2022).
2. Cultural Relevance and Holistic Care
•Aligning with Traditional Practices: Non-pharmacological approaches, such as massage and skin-to-skin contact, often align with traditional Indonesian care practices.
•Holistic Well-being: These methods address not only physical pain but also emotional and psychological distress, promoting relaxation and a sense of control for the patient.
•Involving Family: Techniques often involve family members in the care process, which is culturally important in Indonesia and increases patient satisfaction (Kartika et al., 2024).
3. Patient Autonomy and Self-Care
•Empowerment: Non-drug pain relief techniques, such as breathing exercises or guided imagery, empower patients with self-care strategies to manage their pain independently.
•Improved Quality of Life: These strategies improve comfort levels, particularly for patients with chronic pain or those receiving palliative care (El Geziry et al., 2018).
4. Cost-Effectiveness and Accessibility
•Low-Resource Friendly: Many non-drug pain relief techniques are inexpensive and easy to implement, making them suitable for various healthcare settings across Indonesia, including those with limited resources.
•Reduced Costs: These techniques can reduce the overall burden on the healthcare system by limiting the need for more expensive pharmacological interventions (Tekletsadik et al., 2021).
5. Essential Role of Nurses
•Independent Practice: Nurses can apply many non-drug methods (e.g., repositioning, distraction techniques) independently without waiting for, or in addition to, orders for medication.
•Improved Quality of Care: Training nurses in these techniques enhances their ability to provide comprehensive, humane care, especially for pediatric patients.
In summary, non-drug pain relief techniques are crucial in Indonesia to provide safe, affordable, and culturally appropriate care that addresses the multifaceted nature of pain (Pérez-Pozuelo et al., 2026).
6 Non-Drug Pain Relief Techniques Every Nurse Should Know
Here are the commonly used non-drug pain relief techniques that every nurse should know (El Geziry et al., 2018; Hui, 2025; Stanford Health Care, 2021):
1. Positioning and Mobilization
Often, the simplest intervention is the most effective.
Poor positioning increases pressure on tissues. This causes muscle tension and worsens pain. Correct alignment improves comfort and circulation.
✔️How to apply:
-Use pillows to support joints
-Elevate swollen limbs
-Reposition every 2–3 hours
-Assist early mobilization after surgery
Clinical tip: Always reassess pain 10–15 minutes after repositioning.
2. Cold and Heat Therapy
Temperature therapy is widely used because it is simple and effective.
✔️Cold therapy (ice/cryotherapy)
•Best for:
Swelling; acute injury; inflammation; trauma
•Effects:
Reduces edema; numbs pain receptors
✔️Heat therapy
•Best for:
Muscle stiffness; chronic pain; spasm
•Effects:
Improves blood flow; relaxes muscles
⚠️Safety reminders:
-Wrap packs with cloth
-Limit to 15–20 minutes
-Check skin integrity
3. Relaxation and Breathing Techniques
Pain and anxiety are closely connected. When anxiety rises, pain perception increases.
Simple breathing techniques help calm the nervous system and reduce pain naturally.
✔️Methods:
-Slow deep breathing
-Guided imagery
-Progressive muscle relaxation
-Counting breaths
✔️Useful when:
-Post-operative patients
-Labor pain
-Dressing changes
-IV insertion
Clinical tip: These techniques take less than 5 minutes to teach.
4. Distraction Techniques
Distraction works by shifting attention away from pain signals.
✔️Options:
-Conversation
-Music
-Videos
-Games
-Storytelling
✔️Particularly effective for:
-Children
-Adolescents
-Minor procedures
By diverting the patient’s focus, distraction techniques can help reduce the perception of pain and make the patient feel more comfortable during the procedure or treatment.
5. Massage and Therapeutic Touch
A gentle massage reduces muscle tension and improves relaxation.
✔️Benefits:
-Promotes circulation
-Reduces stiffness
-Provides emotional comfort
✔️Avoid when there is:
-Fracture
-Infection
-Open wound
-Deep Vein Thrombosis (DVT) risk
Clinical tip: Always consider cultural sensitivity and obtain consent.
6. Environmental Comfort Measures
Sometimes pain increases because the environment is stressful.
Simple adjustments can significantly improve comfort.
✔️Some areas for improvement:
-Noise levels
-Lighting
-Temperature
-Privacy
-Family support
These changes cost nothing but have strong effects.
Applying Techniques Across Clinical Settings
Here are some examples of non-drug pain relief techniques commonly used in various clinical settings:
✔️Emergency Department
-Cold packs for trauma
-Distraction while waiting
-Quick positioning
✔️Surgical Ward
-Repositioning
-Breathing exercises
-Early mobilization
✔️Maternity Unit
-Breathing
-Massage
-Relaxation
✔️Pediatric Care
-Play therapy
-Distraction
-Comfort objects
✔️Community Health Centers (Puskesmas)
-Heat therapy
-Education
-Self-care teaching
Clinical tip: Each setting requires flexibility, but the principles remain the same.
Documentation and Evaluation
Non-drug interventions must be documented just like medications.
✔️What to include?
1. Intervention used
2. Time applied
3. Pain score before/after
4. Patient response
✔️Example of SOAP note:
The Subjective, Objective, Assessment, and Plan (SOAP) note is an acronym representing a widely used method of documentation for healthcare providers (Podder et al., 2023).
S: Patient reports pain score 6/10
O: Guarding abdomen
A: Post-operative pain
P: Repositioned + deep breathing; reassessed → pain 3/10
Documentation shows professional accountability and supports quality improvement.
Common Mistakes Nurses Should Avoid
1. Waiting only for medication orders
2. Forgetting reassessment
3. Applying heat or cold for too long
4. Ignoring patient preferences
5. Not documenting interventions
Remember, small actions make big differences!
How to Practice Non-Drug Techniques Safely
To ensure clinical safety and alignment with Indonesian healthcare standards, the following approaches are recommended:
1. Assess pain first — use numeric scales (NRS 0–10) or validated tools
2. Check for red flags — sudden severe pain, neurologic changes, vital sign instability
3. Choose an appropriate intervention — based on patient condition and context
4. Evaluate and document — before and after intervention
5. Escalate to the medical team when pain persists or worsens
This structured approach supports both clinical effectiveness and regulatory compliance.
Conclusion: Small Nursing Actions, Big Patient Impact
Non-drug pain relief techniques remind us of something fundamental about nursing:
Not all healing comes from medication.
Often, it comes from repositioning a pillow, guiding a breath, applying a cold pack, or offering comfort.
These simple, evidence-based interventions are safe, cost-effective, and highly relevant to Indonesian healthcare settings — from tertiary hospitals in Jakarta to remote puskesmas in rural areas.
By mastering non-pharmacological pain management, nurses deliver care that is not only clinical but also compassionate.
And sometimes, that makes all the difference!
Building Competency Through Training
Although these skills seem simple, proper training ensures:
-Correct technique
-Patient safety
-Standardized care
-Higher confidence
Simulation, case scenarios, and digital learning modules help nurses practice decision-making in real-life situations.
Healthcare institutions that regularly train staff in pain management often see:
-Faster recovery
-Higher patient satisfaction
-Reduced medication use
Make a difference today!
References:
1. El Geziry, A., Toble, Y., Al Kadhi, F., & Pervaiz and Mohammad Al Nobani, M. (2018). Non-Pharmacological Pain Management. Pain Management in Special Circumstances. https://doi.org/10.5772/intechopen.79689
2. Fitri, S. Y. R., Rakhmawati, W., Pahria, T., & Hendrawati, S. (2022). Ethnonursing Study of Pain Management in Neonates in Pangandaran, West Java, Indonesia. Pain Management Nursing. https://doi.org/10.1016/j.pmn.2022.10.001
3. Hui, J. L. Q. (2025). Effective Non-Drug Approaches to Pain Management | Parkway Cancer Centre Philippines. Parkway Cancer. https://www.parkwaycancercentre.com/ph/news-events/news-articles/news-articles-details/effective-non-drug-approaches-to-pain-management
4. Kartika, I. R., Rezkiki, F., Febrina, C., & Khairunnisa, C. W. (2024). Pain Management in the Community: The Empowerment of District on Collaboration of Complementary Nursing at Bukittinggi, West Sumatera. Salus Publica: Journal of Community Service, 1(3), 79–85. https://doi.org/10.58905/saluspublica.v1i3.218
5. Pérez-Pozuelo, J. M., Sonsoles Hernández-Iglesias, Mónica Raquel Pereira-Afonso, Checa-Peñalver, A., Inmaculada García-Valdivieso, Ángel López-González, & Sagrario Gómez-Cantarino. (2026). Effectiveness of non-pharmacological methods in reducing pain in pediatric patients and the role of nursing. Systematic review. Frontiers in Pediatrics, 13. https://doi.org/10.3389/fped.2025.1729847
6. Podder, V., Ghassemzadeh, S., & Lew, V. (2023, August 28). SOAP notes. National Library of Medicine; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK482263/
7. Stanford Health Care. (2021). Management of Pain without Medications. Stanford Medicine. https://stanfordhealthcare.org/medical-conditions/pain/pain/treatments/non-pharmacological-pain-management.html
8. Tekletsadik, E. A., Desta, A. A., & Workneh, B. S. (2021). Knowledge, Attitude, and Associated Factors towards Nonpharmacological Pain Management among Nurses Working at Amhara Region Comprehensive Specialized Hospitals, Ethiopia. Critical Care Research and Practice, 2021, 1–11. https://doi.org/10.1155/2021/7374915
9. Tsegaye, D., Yazew, A., Gedfew, M., Yilak, G., & Yalew, Z. M. (2023). Non-Pharmacological Pain Management Practice and Associated Factors among Nurses Working at Comprehensive Specialized Hospitals. SAGE Open Nursing, 9(9). https://doi.org/10.1177/23779608231158979





