Medical Devices in Infection Control: Reducing HAIs in Healthcare

Infection control is one of the most important steps in healthcare risk management. This helps ensure patient safety, protecting them against healthcare associated infections or HAIs. Although hand hygiene or the use of personal protective equipment (PPE) are more familiar, the role of medical devices in infection control is usually neglected.
Healthcare providers understand that the proper handling, sterilization, and use of medical devices—ranging from reusable instruments to advanced monitoring systems—can greatly lower the risk of infections across various healthcare environments.
In this article, we explore how medical devices contribute to infection control and what healthcare professionals can do to minimize infection risks.
Current Statistics on Healthcare Associated Infections (HAIs)
HAIs are among the most prevalent and preventable adverse events in healthcare, posing a serious threat to patient safety, especially in hospitals and ICUs.
Medical devices in infection control play a critical role in reducing HAIs, particularly in high-risk settings where catheters, ventilators, and other invasive devices increase infection risks.
WHO (2024) reports that 1 in 10 patients globally acquires an HAI during hospitalization, with incidence rates significantly higher in low- and middle-income countries and ICU patients.
24% of HAI cases lead to severe complications, with ICU patients facing a 52.3% mortality rate due to infection-related conditions.
Gade et al. (2023) found that device-associated HAIs are the third most common adverse event in healthcare, with ICUs reporting 5 infections per 1,000 patient days, and ventilator-associated pneumonia (VAP) being the most frequent.
Goh et al. (2023) identified Indonesia as having the highest HAI prevalence in Southeast Asia (30.4%), highlighting the need for enhanced infection control measures.
WHO (2024) confirms that infection prevention and control (IPC) interventions can reduce HAIs and antimicrobial resistance by 35-70%, making them both highly effective and cost-saving for healthcare facilities worldwide.
The Role of Medical Devices in Infection Control
While medical devices are important to patient care, without proper attention they can also serve as potential sources of infection.
Here are some ways medical devices contribute to infection control:
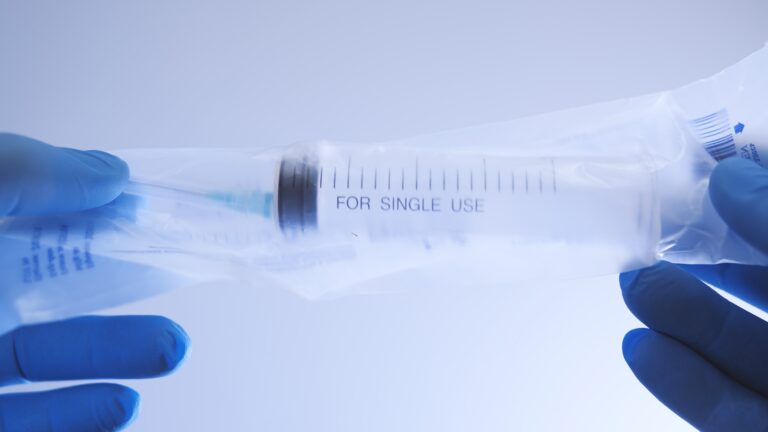
1. Single Use Vs. Reusable Medical Devices
Single-use devices can aid in infection control as the items are thrown away after one use.
Examples: syringes, catheters, and disposable gloves
Reusable medical devices need proper handling, meticulous disinfection, and sterilization to prevent cross-contamination.
Examples: endoscopes, surgical tools, and ventilators
Key Infection Control Measure: Healthcare facilities must follow strict decontamination protocols and regularly audit their sterilization processes to prevent infections from reusable devices.

2. Proper Sterilization & Disinfection of Medical Equipment
Autoclaving: High-pressure steam sterilization for surgical instruments.
Chemical Disinfection: Using antiseptics and disinfectants to eliminate pathogens.
UV Sterilization: Newer technology that uses ultraviolet light to disinfect surfaces and tools.
Key Infection Control Measure: Hospitals should train healthcare workers on the correct cleaning procedures and regularly inspect sterilization equipment to maintain infection-free environments
3. Monitoring & Maintenance of Medical Equipment
Poorly maintained or contaminated medical devices can become breeding grounds for bacteria. Some examples include ventilators, dialysis machines, or IV pumps.
Routine inspections and servicing help ensure devices function properly and do not harbor infectious agents.
Key Infection Control Measure: Implement a preventive maintenance schedule for all medical equipment to minimize infection risks and prolong the lifespan of devices.
Common Healthcare-Associated Infections (HAIs) Linked to Medical Devices
According to the Centers for Disease Control and Prevention, some of the most common HAIs caused by medical devices include:
Infection Type | Medical Device Risk Factor |
Catheter-Associated Urinary Tract Infections (CAUTI) | – Improperly handled urinary catheters |
Ventilator-Associated Pneumonia (VAP) | – Contaminated ventilators & breathing circuits |
Surgical Site Infections (SSI) | – Non-sterile surgical instruments |
Central Line-Associated Bloodstream Infections (CLABSI) | – Poor handling of central venous catheters |
Studies and Examples on Medical Devices in Infection Control
Textiles impregnated with antimicrobial substances in healthcare services: systematic review
Reviews 23 intervention studies
Textiles impregnated with substances like copper, silver, zinc oxide, titanium, and quaternary ammonium compounds are effective in lowering microbial contamination when used by patients, healthcare professionals, and in healthcare environments
Notes concerns regarding microbial resistance and the need for cautious implementation
Potential additional effects of iron chelators on antimicrobial- impregnated central venous catheters
Discusses approaches to incorporate iron chelators into antimicrobial-impregnated central venous catheters to further suppress microbial colonization and biofilm formation in long term central venous catheters
These approaches hold potential for reducing the incidence of catheter-related infections and improving patient outcomes.
Practical recommendations for routine cleaning and disinfection procedures in healthcare institutions: a narrative review
Highlights the need for standardized cleaning processes, appropriate disinfectants, and the use of disposable and reusable cleaning products
Underscores the importance of training healthcare workers on cleaning and disinfection protocols, including regular supervision and team communication
Achieving Zero CAUTIs Through Team Engagement
Alaska Native Medical Center (ANMC), based in Anchorage, recorded a 9% decrease in the standardized infection ratio for catheter-associated urinary tract infections (CAUTI) in 2020, compared to 2019.
ANMC recorded zero CAUTIs from April through December of 2021
Practices include:
- Enhancing training on appropriate and inappropriate indications for catheter placement and the proper technique for catheter placement
- Ensuring appropriate use of urine cultures and the nontreatment of asymptomatic bacteriuria
- Using real-time data surveillance systems that can track every patient with indwelling urinary catheters, giving team members the information needed for monitoring
Xenco Medical’s plastic-based Cervical Interbody System
Xenco Medical developed single-use, disposable spinal surgery instruments made from reinforced polymer, thereby eliminating any chance of infection due to reused, improperly sterilized instruments.
First used by Dr. Nick Shamie on July 13, 2015 in UCLA
Best Practices for Infection Control Using Medical Devices

1. Train Healthcare Workers on Proper Handling
Educate staff on infection control protocols related to medical devices (Centers for Disease Control and Prevention, 2024).
Conduct regular audits and training to reinforce best practices.
Check our blog on the importance of infection control training to learn more.
2. Follow Manufacturer’s Guidelines
Each medical device has specific sterilization and maintenance instructions.
Adhering to manufacturer recommendations ensures devices are used safely and effectively (Altayyar, 2020).
3. Implement Digital Tracking for Medical Equipment
Use RFID or barcode tracking to monitor device usage and sterilization history (Kusuda et al., 2024).
Prevents accidental reuse of contaminated or expired medical tools.
4. Adopt Advanced Infection Control Technologies
AI-powered hygiene monitoring can help detect improper sterilization (Godbole et al., 2025).
Automated disinfection using UV light reduces contamination risks in healthcare environments.
Example: U.S. Germitec’s UV-C–based disinfection system offers a rapid and efficient alternative to chemical-based sterilization, specifically designed for non-lumen ultrasound probes
Advancements in nanotechnology have led to the development of antimicrobial coatings for medical devices (Suresh kumar Mondal et al., 2024)
Examples: Copper nanoparticles for coating medical devices, Hybrid nanoparticles and nanocomposites to coat medical implants
5. Policy and Regulation
Implementing robust infection control policies and adhering to regulatory standards are essential components of effective medical device management.
In Indonesia, the control of infections related to medical devices is regulated by various agencies and regulations that ensure that the practices of using and maintaining medical devices meet high safety and effectiveness standards. This regulation involves collaboration between the Ministry of Health, the Food and Drug Monitoring Agency (BPOM), and other relevant institutions.
Here are some of the main aspects of the policies and regulations related to infection control in medical devices in Indonesia:
1. Ministry of Health Regulations
The Ministry of Health of the Republic of Indonesia issues various regulations and guidelines governing the use and maintenance of health devices. This includes sterilization and disinfection of medical devices to prevent the spread of infections.
2. BPOM
The Food and Drug Monitoring Agency is responsible for supervising health devices circulating in Indonesia. BPOM regulates the registration, distribution, and supervision of medical devices to ensure that they meet established safety and health standards.
3. SNI (Indonesian National Standard)
The Indonesian National Standard (SNI) sets quality and safety standards for medical devices, including requirements for sterilization and disinfection. The implementation of SNI aims to ensure that all medical devices used in health facilities undergo proper cleaning and maintenance processes to prevent infection.
4. Hospital Accreditation
The Hospital Accreditation Commission (KARS) is an agency that evaluates and accredits hospitals in Indonesia. One of the aspects assessed is infection control, including the management and maintenance of medical devices.
5. Training and Education
Regulation in Indonesia also emphasizes the importance of training and education for healthcare workers. This should include the sterile and hygienic use and maintenance of medical devices to prevent the transmission of infections.
6. Monitoring and Reporting
Health facilities are required to monitor and report every infection event related to medical devices to local health authorities. This information is used to analyze and improve infection control strategies.
The implementation of these policies and regulations is key to ensuring that medical devices do not become a source of infection transmission in healthcare facilities. Moreover, to ensure the safety and quality of healthcare services in Indonesia.
6. Patient Education
The CDC emphasizes that informed patients can actively reduce their risk of HAIs by following proper hygiene, ensuring safe medical device use, and understanding infection control measures.
For detailed patient safety guidelines and tips on infection prevention, visit the CDC’s official Patient Safety page: 👉 CDC Tips for Being a Safe Patient
Moreover, the CDC provides detailed guidelines on infection control and disinfection for all healthcare settings.
To access the latest infection control recommendations, visit: 👉 CDC Infection Control Guidelines
The Association for Professionals in Infection Control and Epidemiology, Inc. have also outlined the basics in educating patients on infection control.
Visit their site here 👉 Educate Your Patients
Medical devices are essential in modern healthcare, but improper handling, maintenance, and sterilization can increase the risk of healthcare-associated infections (HAIs).
The risk of infections can be mitigated by enforcing strict infection control policies, training healthcare personnel, and using new technology.
📌 Want to enhance your infection control knowledge?
Enroll in Zafyre’s Infection Control & Prevention Course and earn 5 SKP points while mastering the best practices for healthcare risk management.
References:
A. Journal Articles
- Altayyar, S. S. (2020). The Essential Principles of Safety and Effectiveness for Medical Devices and the Role of Standards. Medical Devices: Evidence and Research, Volume 13, 49–55. https://doi.org/10.2147/mder.s235467
- Assadian, O., Harbarth, S., Vos, M., Knobloch, J. K., Asensio, A., & Widmer, A. F. (2021). Practical recommendations for routine cleaning and disinfection procedures in healthcare institutions: a narrative review. Journal of Hospital Infection, 113. https://doi.org/10.1016/j.jhin.2021.03.010
- Gade, N., Burri, R., Sujiv, A., Mishra, M., Pradeep, B. E., Debaje, H., Sable, T., & Kaur, A. (2023). Promoting Patient Safety: Exploring Device-Associated Healthcare Infections and Antimicrobial Susceptibility Pattern in a Multidisciplinary Intensive Care Units. Cureus, 15(12). https://doi.org/10.7759/cureus.50232
- Godbole, A. A., Paras, N., Mehra, M., Banerjee, S., Roy, P., Deb, N., & Sarang Jagtap. (2025). Enhancing Infection Control in ICUS Through AI: A Literature Review. Health Science Reports, 8(1). https://doi.org/10.1002/hsr2.70288
- Goh, L. P. W., Marbawi, H., Goh, S. M., Bin Abdul Asis, A. K., & Gansau, J. A. (2023). The prevalence of hospital-acquired infections in Southeast Asia (1990-2022). The Journal of Infection in Developing Countries, 17(02), 139–146. https://doi.org/10.3855/jidc.17135
- Itoh, K., Hiroshi Tsutani, Yasuhiko Mitsuke, & Iwasaki, H. (2023). Potential additional effects of iron chelators on antimicrobial- impregnated central venous catheters. Frontiers in Microbiology, 14. https://doi.org/10.3389/fmicb.2023.1210747
- Kusuda, K., Yamashita, K., Morishita, E., Ishibashi, N., Shiraishi, Y., & Yamaguchi, H. (2024). Comparison of Reading Times of RFID-Tagged and Barcode-Engraved Surgical Instruments. Journal of Surgical Research, 304, 121–125. https://doi.org/10.1016/j.jss.2024.09.087
- Schneider, G., Leticia Genova Vieira, Félix, E., Lopes, F., Watanabe, E., Denise de Andrade, & Cristina, R. (2023). Textiles impregnated with antimicrobial substances in healthcare services: systematic review. Frontiers in Public Health, 11. https://doi.org/10.3389/fpubh.2023.1130829
- Suresh kumar Mondal, Chakraborty, S., Manna, S., & Mandal, S. M. (2024). Antimicrobial Nanoparticles: Current Landscape and Future Challenges. RSC Pharmaceutics, 1. https://doi.org/10.1039/d4pm00032c
B. Other References
- American Hospital Association. (2020). Alaska Native Medical Center: Achieving Zero CAUTIs Through Team Engagement | AHA. American Hospital Association. https://www.aha.org/alaska-native-medical-center-achieving-zero-cautis-through-team-engagement
- Centers for Disease Control and Prevention. (2024, May 10). CDC’s Core Infection Prevention and Control Practices for Safe Healthcare Delivery in All Settings. Infection Control. https://www.cdc.gov/infection-control/hcp/core-practices/index.html
- Centers for Disease Control and Prevention. (2024, May 15). Healthcare-Associated Infections (HAIs). Healthcare-Associated Infections (HAIs). https://www.cdc.gov/healthcare-associated-infections/index.html
- Infection Control Today. (2015, July 18). Xenco Medical Announces Surgeon Performs Spine Surgery Using Disposable Plastic Surgical Instruments. Infection Control Today. https://www.infectioncontroltoday.com/view/xenco-medical-announces-surgeon-peorms-spine-surgery-using-disposable-plastic-surgical
- US Food and Drug Administration. (2018, September 27). Reprocessing of Reusable Medical Devices. U.S. Food and Drug Administration. https://www.fda.gov/medical-devices/device-advice-comprehensive-regulatory-assistance/reprocessing-reusable-medical-devices-information-manufacturers





