6 Life-saving ECG Rhythms Every Indonesian Nurse Must Know

ECG (Electrocardiogram) interpretation is no longer just a critical care skill—it’s a must-have competency for every nurse in Indonesia, especially with the increasing rates of heart disease, hypertension, and stroke in the country. Recognizing life-threatening ECG rhythms is essential!
As Indonesia continues to expand its National Health Insurance (JKN) coverage and improve access to primary and emergency care, nurses are now expected to recognize life-threatening ECG ryhthms early, even in puskesmas, rural clinics, and ambulances.
Whether you’re a clinical nurse in a government hospital, a nursing student preparing for Uji Kompetensi (UKOM), or part of the growing telemedicine movement, here are 6 core ECG rhythms every Indonesian nurse should understand—and why they matter for patient safety and professional growth.
1. Normal Sinus Rhythm (NSR)
❓What it is: The healthy baseline rhythm from the heart’s SA node.
✅ Key Features (Burns & Buttner, 2024) :
Regular rhythm at a rate of 60-100 bpm (or age-appropriate rate in children)
QRS complex: preceded by a normal P wave; < 100 ms wide (unless co-existent interventricular conduction delay present)
Normal P wave axis: P waves are upright in leads I and II, inverted in aVR
PR interval: remains constant (0.12–0.20 sec)
QRS duration: < 0.12 sec

🩺Why it matters:
NSR is the rhythm against which all others are compared as a baseline. Nurses must first recognize a normal pattern before identifying any abnormal or dangerous changes.
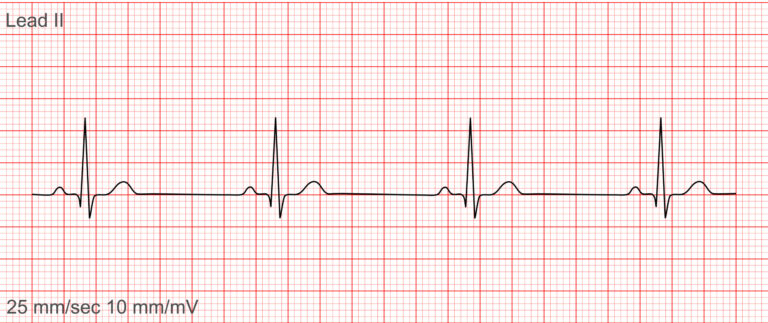
2. Sinus Bradycardia
❓What it is: A slow heart rhythm that originates from the SA node.
✅ Key Features (Livingston, 2024):
Rate: < 60 beats per minute
Rhythm: Regular
P waves: Upright, consistent, and normal in morphology and duration, indicating normal sinus node function
PR interval: 0.12-0.20 seconds
QRS complex: < 0.12 seconds in width, and consistent in morphology, meaning the ventricles are contracting in response to the sinus node signal
🩺Why it matters:
Sinus bradycardia is the ECG rhythm that can be normal among athletes, but in elderly patients or those on beta-blockers or digitalis (still commonly used in Indonesia), it may signal compromised perfusion.
⚠️ Watch out for hypotension, decreased consciousness, or fainting.
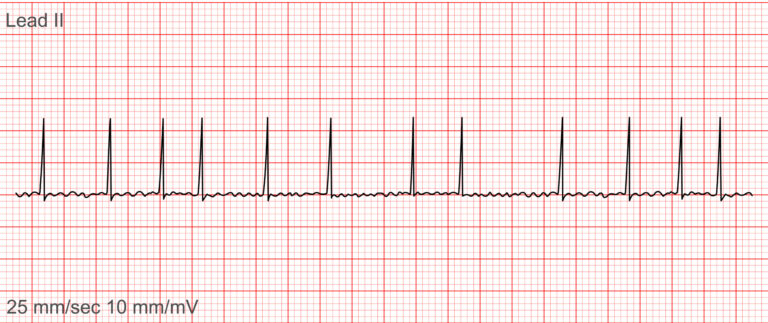
3. Atrial Fibrillation (AFib)
❓What it is: An irregular and often very rapid heart rhythm from the atrial chambers of the heart.
✅ Key Features (Burns & Buttner, 2024):
Irregularly irregular rhythm
No P waves
Absence of an isoelectric baseline
Variable ventricular rate
QRS complexes: usually < 120ms (unless pre-existing bundle branch block, accessory pathway, or rate-related aberrant conduction)
Fibrillatory waves may be present and can be either fine (amplitude < 0.5mm) or coarse (amplitude > 0.5mm)
Fibrillatory waves may mimic P waves, leading to misdiagnosis
🩺Why it matters:
AFib is on the rise in Indonesia. This is especially true for patients with uncontrolled hypertension, diabetes, or thyroid disorders. It is associated with stroke, which is one of the leading causes of mortality and disability in Indonesia. Nurses must identify it early for immediate referral and treatment.
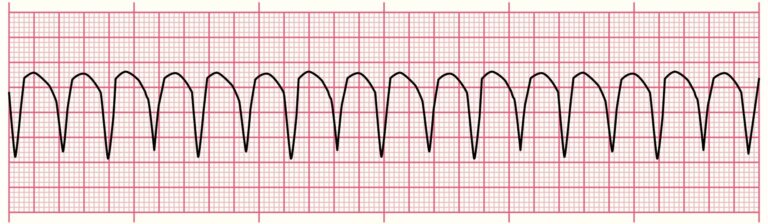
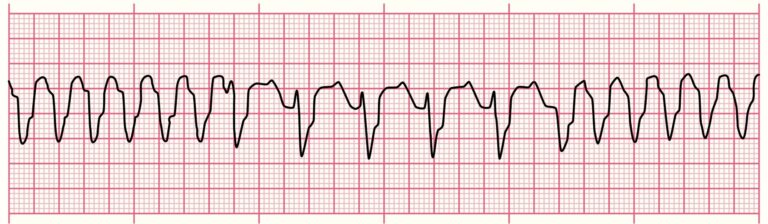
4. Ventricular Tachycardia (VTach)
❓What it is: A rapid, dangerous ECG rhythm from the ventricles.
✅ Key Features (Foth et. al., 2023 and Mitchell, 2024) :
Wide QRS complexes: The QRS complex is broader than normal, typically lasting more than 0.12 seconds (120 milliseconds).
Rapid heart rate: Generally above 120 beats per minute
Absence of P waves: P waves may be present (not related to the QRS complexes), or may be absent
Other ECG features that may be present during VT:
–Atrioventricular (AV) dissociation: The atria and ventricles beat independently of each other.
–Fusion or capture beats: Occasional beats where the normal heart rhythm briefly takes over during VT.
🩺Why it matters:
⚠️ Emergency Alert!
VT can quickly deteriorate into ventricular fibrillation and cardiac arrest, which means every minute counts. Nurses, even those outside the ICU, must be able to initiate Code Blue protocols, start high-quality CPR, and assist in early defibrillation using an AED or manual defibrillator.
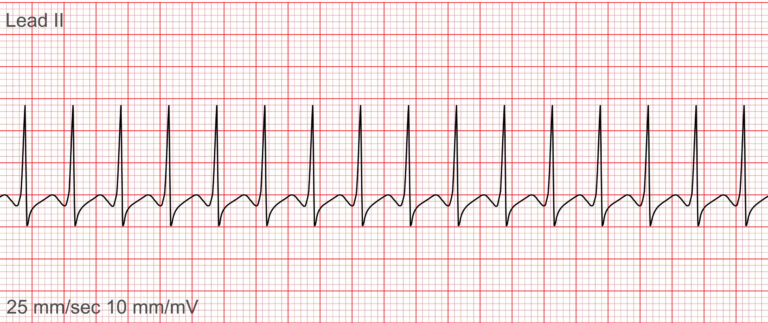
5. Supraventricular Tachycardia (SVT)
❓What it is: The term supraventricular tachycardia (SVT) refers to any tachydysrhythmia arising from above the level of the Bundle of His, and encompasses regular atrial, irregular atrial, and regular atrioventricular tachycardias (Burns & Buttner, 2024).
✅ Key Features (Patti & Ashurst, 2025):
Heart Rate: Exceeding 100 bpm, typically 150–220 bpm
Rhythm: Regular
P waves: Often hidden within preceding T waves or absent
QRS: Narrow (< 0.12 sec) unless pre-existing bundle branch block
Onset and termination: Sudden
🩺Why it matters:
SVT can cause severe hypotension, chest pain, or syncope, especially in patients with underlying heart disease. Even though SVT is often less immediately fatal than VT, delayed treatment can cause rapid decompensation. Nurses should be familiar with vagal maneuvers (e.g., Valsalva) and be ready to assist with adenosine administration or synchronized cardioversion per ACLS guidelines.
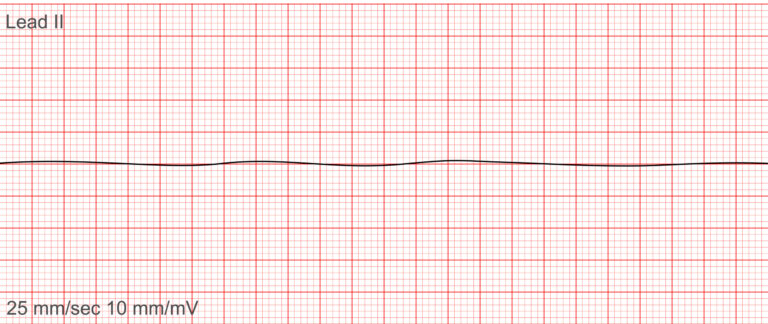
6. Asystole (Flatline)
❓What it is: Complete cardiac standstill—no electrical activity.
✅ Key Features (Ramadan, 2024):
No QRS complexes
Flatline ECG
Possibly faint P waves early on
No pulse, no heartbeat
🩺Why it matters:
⚠️ Immediate action is needed!
Begin high-quality CPR immediately, give epinephrine, and identify any reversible causes (the H’s and T’s). Defibrillation is not effective. This rhythm is often misread—make sure the leads are connected and the ECG machine is functional before confirming asystole.

Why ECG Skills Are Now Essential for Indonesian Nurses
With the Ministry of Health’s initiative to digitize healthcare and expand critical care networks (Jejaring Rujukan Nasional), nurses are increasingly expected to identify abnormal ECG rhythms early during cardiac triage and emergency referrals.
💡 Did you know?
Many nurses in ambulances and rural clinics now use portable ECG devices to send readings to cardiologists via tele-ECG systems supported by BPJS or SmartCity initiatives.
ECG interpretation allows nurses to:
1. Detect heart attacks, arrhythmias, and electrolyte imbalances
2. Respond to emergencies faster, especially in disaster zones or remote areas
3. Support physician decision-making with accurate monitoring
4. Improve patient safety, especially during transfers and pre-hospital care
5. Prepare for UKOM and meet CPD (Continuing Professional Development) requirements
📚 Master ECG Interpretation with Zafyre's Online Course
Ready to boost your clinical confidence?
Zafyre offers an ECG Interpretation Course designed specifically for Indonesian nurses.
✅ Whether you’re working in RSUD, puskesmas, emergency ambulance teams, or ICU, this course will help you:
Analyze ECG grids, waveforms, intervals, and cardiac axis
Identify key ECG rhythms like VTach and AFib
Interpret ECGs in real clinical scenarios
Earn a certificate accredited by KEMENKES
🎓 Also suitable for UKOM preparation and continuing professional education!
👉 Enroll Now | Learn anytime, anywhere!
Bonus: Trending Tip for Indonesian Nurses
💬 Many hospitals in Indonesia now prioritize nurses with ECG skills for rotation into IGD and ICU. ECG interpretation isn’t just about saving lives—it’s a career booster!
References:
- Burns, E., & Buttner, R. (2024, October 8). Normal sinus rhythm. Life in the Fast Lane • LITFL • Medical Blog. https://litfl.com/normal-sinus-rhythm-ecg-library/
- Burns, E., & Buttner, R. (2024, October 8). Atrial Fibrillation • LITFL Medical Blog • ECG Library Diagnosis. Life in the Fast Lane • LITFL • Medical Blog. https://litfl.com/atrial-fibrillation-ecg-library/
- Burns, E., & Buttner, R. (2024, October 8). Supraventricular Tachycardia (SVT) • LITFL • ECG Library Diagnosis. Life in the Fast Lane • LITFL • Medical Blog. https://litfl.com/supraventricular-tachycardia-svt-ecg-library/
- Foth, C., Gangwani, M. K., & Alvey, H. (2023, July 30). Ventricular Tachycardia. Nih.gov; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK532954/
- Livingston, M. (2024). Sinus Bradycardia. EMedicine. https://emedicine.medscape.com/article/760220-overview
- Mitchell, L. B. (2024, September). Ventricular Tachycardia (VT) – Cardiovascular Disorders. MSD Manual Professional Edition. https://www.msdmanuals.com/professional/cardiovascular-disorders/specific-cardiac-arrhythmias/ventricular-tachycardia-vt
- Patti, L., & Ashurst, J. V. (2025). Supraventricular Tachycardia. Nih.gov; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK441972/
- Ramadan, M. M. (2024). Replacing the term “Asystole” with “Absent Electrical Activity.” Resuscitation Plus, 19, 100682–100682. https://doi.org/10.1016/j.resplu.2024.100682
- Sattar, Y., & Chhabra, L. (2023). Electrocardiogram. National Library of Medicine; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK549803/
- The Importance Of ECG Interpretation In Critical Care Settings | Tricog Health. (2024, June 24). Tricog Health. https://www.tricog.com/the-importance-of-ecg-interpretation-in-critical-care-settings/





